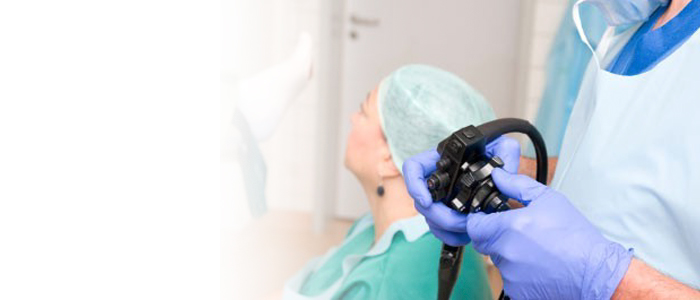
Upper endoscopy is a procedure allowing your gastroenterologist to examine the esophagus , stomach, and duodenum using a thin, flexible tube called an endoscope through which the lining of the esophagus, stomach, and duodenum can be viewed.
Prior to scheduling the procedure, you should let us know about any medications you are taking. as well as any allergies, and all known health problems. This information will help your doctor determine whether the patient may need antibiotics prior to the procedure, and what potential medications should not be used during the exam because of the patient’s allergies.
Why you should have an endoscopy
Upper endoscopy performed in order to evaluate possible problems with your esophagus, stomach or duodenum, and evaluate any symptoms such as upper abdominal pain, nausea or vomiting, difficulty in swallowing, or intestinal bleeding anemia. Upper endoscopy is far more accurate than X-ray for detecting inflammation or smaller abnormalities such as ulcers or tumors within the reach of the instrument. Its other major advantage over X-ray is the ability to perform biopsies (obtain small pieces of tissue) or cytology (obtain some cells with a fine brush) for microscopic examination to determine the nature of the abnormality and whether any abnormality is benign or malignant (cancerous).
Biopsies are taken for many reasons and may not mean that cancer is suspected. Upper endoscopy also can be used to treat many conditions within its reach. The endoscope’s channels permit passage of accessory instruments enabling the examiner to treat many of the conditions such as stretching areas of narrowing (strictures, Schatzki ring), removal of benign growths such as polyps, retrieving accidentally swallowed objects, or treating upper gastrointestinal bleeding, as seen in ulcers tears of the lining. These capabilities have markedly reduced the need for transfusions or surgery
Heartburn:Foods to Eat, Foods to Avoid
Before the procedure we will discuss with you why the procedure is being done, whether there are alternative procedures or tests, and what possible complications may result from the endoscopy. Before the exam you may have your throat sprayed with a numbing solution and will probably be given a sedating and pain alleviating medication through a vein. You will be relaxed after receiving this medication and you may even go to sleep. This form of sedation is called conscious sedation and is usually administered by a nurse who monitors you during the entire procedure.
What You Can Expect
After you are sedated while lying on your left side the flexible video endoscope, the thickness of a small finger, is passed through the mouth into the esophagus, stomach, and duodenum. This procedure will NOT interfere with your breathing. Most patients experience only minimal discomfort during the test and many sleep throughout the entire procedure using conscious sedation. Deep sedation ensures that you feel no discomfort during the entire procedure.
What happens after the endoscopy?
After the test the patient will be observed and monitored by a qualified individual in the endoscopy or a recovery area until a significant portion of the medication has worn off. Occasionally a patient is left with a mild sore throat, which promptly responds to saline gargles, or a feeling of distention from the air that was used during the procedure. Both problems are mild and transient. When fully recovered, the patient will be instructed when to resume their usual diet (probably within a few hours) and the patient’s driver will be allowed to take the patient home. (Because of the use of sedation, most facilities mandate that the patient be taken by a driver and not drive, handle machinery, or make important decisions for the remainder of the day.)
When do I get my results?
Under most circumstances, the examining physician will inform the patient of the test results or the probable findings prior to discharge from the recovery area. The results of biopsies or cytology usually take 72-96 hours and the doctor may only give the patient a presumptive diagnosis pending the definitive one, after the microscopic examination.
What are the risks of endoscopy?
Endoscopy is a safe procedure and when performed by a physician with specialized training in these procedures, the complications are extremely rare. They may include localized irritation of the vein where the medication was administered, reaction to the medication or sedatives used, complications from pre-existing heart, lung, or liver disease, bleeding may occur at the site of a biopsy or removal of a polyp (which if it occurs is almost always minor and rarely requires transfusions or surgery). Major complications such as perforation (punching a hole through the esophagus, stomach, or duodenum) are rare but usually require surgical repair.
What if there are still remaining questions about endoscopy?
If the patient has any questions about their need for this exam, the cost of this procedure and whether it is covered by the patient’s insurance, methods of billing, or any concerns about this exam, speak to the doctor or his staff about them. Most endoscopists are highly trained specialists and will be happy to discuss their qualifications and answer any questions.
What preparation is required?
Your doctor will tell you what dietary restrictions to follow and what cleansing routine to use. Be sure to follow your doctor’s instructions carefully.
Can I take my current medications?
Most medications can be continued as usual, but some medications can interfere with the preparation or the examination. Inform your doctor about medications you’re taking, particularly aspirin products, arthritis medications, anticoagulants (blood thinners), insulin or iron products. Also, be sure to mention allergies you have to medications.
Alert your doctor if you require antibiotics prior to dental procedures, because you might need antibiotics before a endoscopy as well.
What happens during endoscopy?
endoscopy is well-tolerated and rarely causes much pain. You might feel pressure, bloating or cramping during the procedure. Your doctor might give you a sedative to help you relax and better tolerate any discomfort.
What if the endoscopy shows something abnormal?
If your doctor thinks an area needs further evaluation, he or she might pass an instrument through the endoscope to obtain a biopsy (a sample of the lining) to be analyzed. Biopsies are used to identify many conditions, and your doctor might order one even if he or she doesn’t suspect cancer. If endoscopy is being performed to identify sites of bleeding, your doctor might control the bleeding through the colonoscope by injecting medications or by coagulation (sealing off bleeding vessels with heat treatment). Your doctor might also find polyps during endoscopy, and he or she will most likely remove them during the examination. These procedures don’t usually cause any pain.
What are polyps and why are they removed?
Polyps are abnormal growths in the lining that are usually benign (noncancerous). They vary in size from a tiny dot to several inches. Your doctor can’t always tell a benign polyp from a malignant (cancerous) polyp by its outer appearance, so he or she might send removed polyps for analysis. Because cancer begins in polyps, removing them is an important means of preventing cancers.
How are polyps removed?
Your doctor might destroy tiny polyps by fulguration (burning) or by removing them with wire loops called snares or with biopsy instruments. Your doctor might use a technique called “snare polypectomy” to remove larger polyps. That technique involves passing a wire loop through the colonoscope and removing the polyp from the intestinal wall using an electrical current. You should feel no pain during the polypectomy.
What happens after a endoscopy?
Your physician will explain the results of the examination to you, although you’ll probably have to wait for the results of any biopsies performed.
If you have been given sedatives during the procedure, someone must drive you home and stay with you. Even if you feel alert after the procedure, your judgment and reflexes could be impaired for the rest of the day. You might have some cramping or bloating because of the air introduced into the colon during the examination. This should disappear quickly when you pass gas.
You should be able to eat after the examination, but your doctor might restrict your diet and activities, especially after polypectomy.
What are the possible complications of endoscopy?
endoscopy and polypectomy are generally safe when performed by doctors who have been specially trained and are experienced in these procedures.
One possible complication is a perforation, or tear, through the bowel wall that could require surgery. Bleeding might occur at the site of biopsy or polypectomy, but it’s usually minor. Bleeding can stop on its own or be controlled through the colonoscope; it rarely requires follow-up treatment. Some patients might have a reaction to the sedatives or complications from heart or lung disease.
Although complications after endoscopy are uncommon, it’s important to recognize early signs of possible complications. Contact your doctor if you notice severe abdominal pain, fever and chills, or rectal bleeding of more than one-half cup. Note that bleeding can occur several days after the procedure.